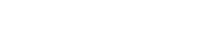Meet your Rx benefits advocate
Remedy Analytics is a team of PBM professionals, clinicians, actuaries and data scientists who provide full-service consulting backed by powerful analytics to unlock the full potential of your Rx benefits.

In the Rx space, there’s no one else quite like Remedy
To truly understand how your plan is performing and where it needs to change, you need a dedicated team, backed by powerful technology.
Meet the Team
Leadership

Kerry Carmichael
Managing SVP Pharmacy Consulting Services, Employee Benefits Leader

Joshua Halperin, PharmD
SVP Pharmacy Consulting Services, Clinical Leader

Steve Maike, R.Ph.
Executive Advisor
Client Engagement

Sharee Bowsher
Senior Director Client Engagement & Business Development

Rosa Bucio
Senior Account Coordinator

Whitney Burkhalter, MBA, PHR
Senior Account Manager

Michelle Cartagena
Senior Account Coordinator

Moriah Comeau
Account Coordinator
Remedy is the new industry leader for management of pharmacy benefits
Our Core Values
Advocacy
We were founded on the guiding principle to help payers navigate the complex and ever-changing prescription drug space. Our relentless endeavor to obtain the best possible outcome for our clients comes from a belief that PBM contracts should be forthright and transparent. We think that’s worth fighting for.
Clarity
We believe in providing clarity in an otherwise convoluted industry. This also means that we admit when we don’t know something and commit to finding the answer. Such transparency allows us to not only identify the problems but also reveal the opportunities.
Innovation
It’s in our DNA to create. We’ve built PharmaLogic®, an industry-changing analytics platform, because we knew only through technology could we do it better. As a thought leader in the prescription benefits space, we continue to innovate by constantly iterating the software and by staying curious.
Impact
Inefficiencies and rising costs in the U.S. pharmacy industry have a direct impact on people and their health. It’s why plan sponsors strive to provide the best coverage for the best price. It’s also why we are committed to supporting them. Together, we can help revolutionize the management of pharmacy benefits.
Integrity
We foster trust in our clients by delivering data-backed services that are both unbiased and hard-hitting. Our solutions work to benefit plan sponsors and their members first.
Engagement
Our team fully engages with each client, learning their pain points and working closely to design their goals. Plan sponsors benefit from frequent touchpoints across many disciplines: PBM advisors, actuaries, clinicians and data analysts give you a 360-degree Rx solution.
Advocacy
We were founded on the guiding principle to help payers navigate the complex and ever-changing prescription drug space. Our relentless endeavor to obtain the best possible outcome for our clients comes from a belief that PBM contracts should be forthright and transparent. We think that’s worth fighting for.
Innovation
It’s in our DNA to create. We’ve built PharmaLogic®, an industry-changing analytics platform, because we knew only through technology could we do it better. As a thought leader in the prescription benefits space, we continue to innovate by constantly iterating the software and by staying curious.
Clarity
We believe in providing clarity in an otherwise convoluted industry. This also means that we admit when we don’t know something and commit to finding the answer. Such transparency allows us to not only identify the problems but also reveal the opportunities.
Impact
Inefficiencies and rising costs in the U.S. pharmacy industry have a direct impact on people and their health. It’s why plan sponsors strive to provide the best coverage for the best price. It’s also why we are committed to supporting them. Together, we can help revolutionize the management of pharmacy benefits.
Integrity
We foster trust in our clients by delivering data-backed services that are both unbiased and hard-hitting. Our solutions work to benefit plan sponsors and their members first.
Engagement
Our team fully engages with each client, learning their pain points and working closely to design their goals. Plan sponsors benefit from frequent touchpoints across many disciplines: PBM advisors, actuaries, clinicians and data analysts give you a 360-degree Rx solution.

Have a question?
We have answers.
What role does a PBM perform?
A PBM — prescription benefits manager — facilitates the processing, dispensing and payment of prescription drugs on behalf of employers and other plan sponsors so that employees can get their prescriptions filled seamlessly at a variety of locations, such as a local pharmacy, chain pharmacy or via mail-order service. Simply, a PBM plays an essential role in the Rx landscape. There are many options for PBM vendors, all with varying strengths, weaknesses and capabilities. Remedy assists employers, TPAs, health systems and other plan sponsors with the vetting, procurement, and contracting with a PBM. Remedy also provides frequent monitoring throughout the year, auditing and reporting of PBM performance and adherence to the contract from an agnostic, unbiased perspective.
How do PBMs price drugs and why is it so difficult to grasp?
How PBMs charge for drugs can be extremely complicated, especially for those who don’t have the specialized experience and analytics to understand the complex process. Simplistically, PBMs price drugs based upon different pricing models such as AWP, NADAC, WAC, and/or MAC. The calculations are anything but simple, given all the complexity of the price model (e.g. discounted aggregate averages, cost-plus reimbursement, acquisition cost plus, etc.), the frequent pricing changes (which can be daily, weekly, monthly for any given drug), and the vagaries of determining the disposition of any given claim within the PBM’s pricing model (e.g. brand vs generic, biosimilar vs specialty). This labyrinth pricing is so challenging that even the most alert payer may not know if the cost of a medication it bought is contractually correct, let alone priced competitively.
How does Remedy solve for this problem?
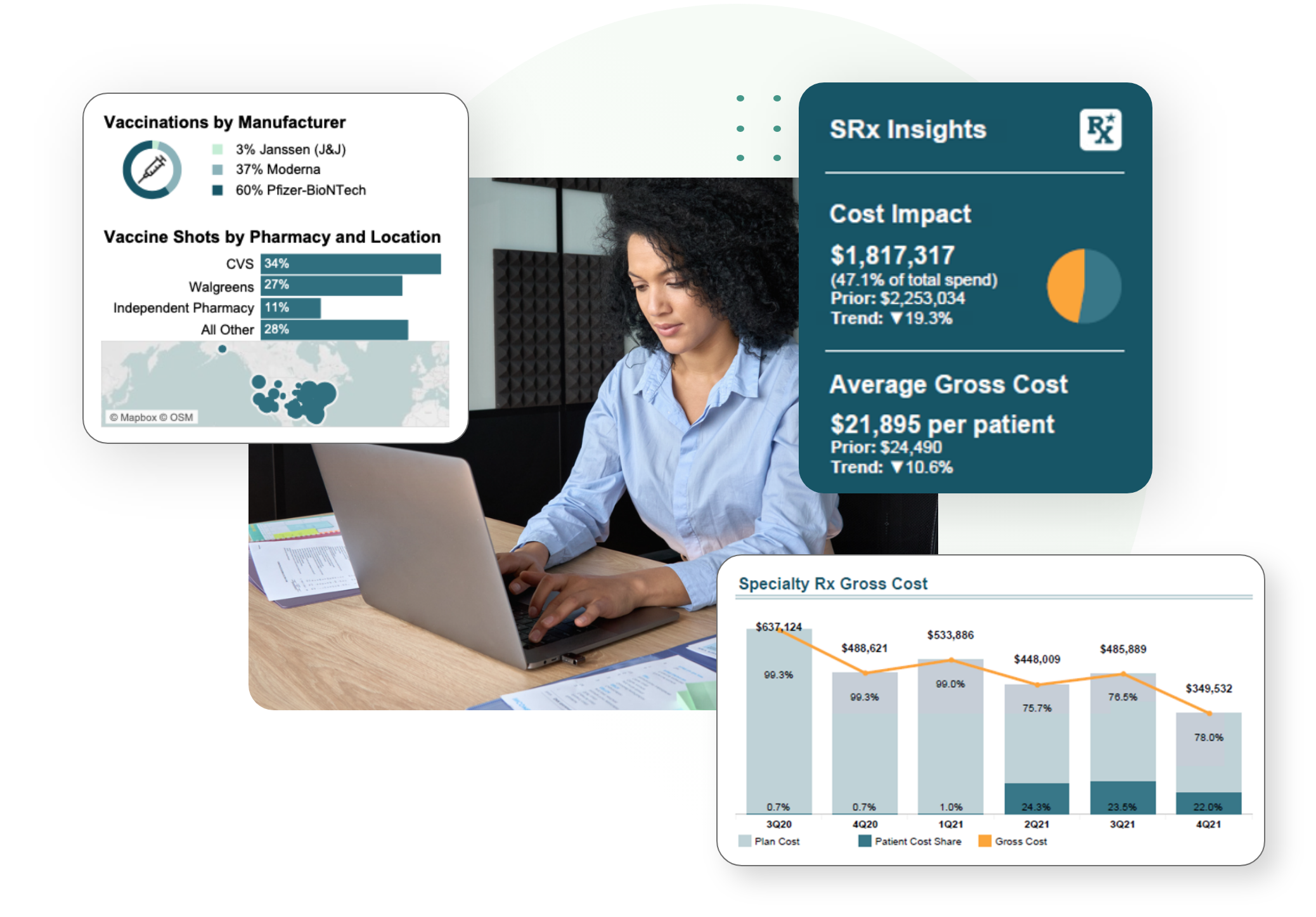
Our proprietary technology, PharmaLogic®, empowers Remedy to see your Rx program in a fundamentally different way than others can. This unparalleled insight allows us to first make sure your contract is definitionally clear and market-fair. Then, using PharmaLogic®, Remedy analyzes each claim down to its granular level in order to optimize both unit cost and drug mix. PharmaLogic® analytics is also used to provide deep dives into pharmacy data to understand spend and trend, along with identifying recommendations and program solutions to lower costs.
What are the typical contractual savings that Remedy finds?
Savings vary, but historically they average between 10% and 20% per year. In some cases, they can reach well over 30%. Depending on your member population, that can translate to millions of dollars saved each year.
Does the Remedy solution impact the benefit plan or copay to the employee?
Plans can achieve savings through a combination of lowering unit costs as well as optimizing drug utilization and mix. Unit cost savings are achieved from aggressive contract negotiations and procurement with the PBMs. This strategy does not require a plan or copay change. Drug utilization savings are typically achieved from enhancements to clinical programs and formulary strategies and may require certain plan changes. Remedy works with clients to understand their unique goals and benefits philosophy and can provide clients with either unit cost savings or drug mix savings (or both) depending on a client’s appetite for change.
Are we required to make a PBM change with Remedy?
No. Remedy can work with any PBM or carrier, including a client’s current provider. That said, if a plan sponsor desires a change, we can walk you through the process – from RFP to onboarding – so that any disruptions are minimal and the process goes smoothly.
Does Remedy continue to work with us after the initial analysis?
Yes. Our Client Engagement team works closely with plan sponsors beyond the initial claims data analysis, including conducting an RFP, securing the improved PBM contract, providing regular pharmacy insights via our analytics and reporting, auditing and contract oversight, ongoing PBM relationship support, and more. Our PharmaLogic® Actionboards provide plan sponsors with actionable data to make intelligent decisions for your Rx spending year-round.
How is Remedy different from the consulting firm we use?
It’s been our experience that others do not have the combination of deep industry knowledge and analytics technology that Remedy has. The Remedy team collectively has hundreds of years of pharmacy benefit experience, and many of our teammates have dedicated their entire careers to understanding PBMs and pharmacy benefits. Our PharmaLogic® technology allow us to view each pharmacy claim at the granular level, and we have created a series of Actionboards to help clients clearly and concisely understand what is going on below the waterline in their pharmacy benefit and how a plan sponsor can make meaningful changes to lower spend and trend.
Is Remedy an auditing company?
Remedy is a pharmacy benefit consulting and analytics company. Conducting audits of a PBM contract on behalf of our clients is one of the many services that we provide. Remedy analyzes up to 600 data points for each claim to determine exactly how the PBMs are performing.
Does Remedy outsource or subcontract the work?
No. All of our core services are provided in-house. In addition to employing our own engineers to build and innovate on the PharmaLogic® platform, Remedy has a team of pharmacists, actuaries and PBM-industry professionals who put the analytics in context for the client. Together they are an ever-ready resource for our clients’ HR and benefits departments to best help them understand how their investment in their employees is being used and how they could further tweak their plan going forward.
In one sentence, how is Remedy different from everyone else?
Through technology and data-driven insight, Remedy enables plan sponsors to maximize their unit cost savings and optimize their drug mix.
When is the right time to review our current PBM program?
At any time. Remedy’s technology and comprehensive solutions can be utilized at any time in your benefits cycle. The results of our findings remain the same; our strategy to secure your savings changes depending on whether you choose to remain with the incumbent or go to market through an RFP.
Who can take advantage of Remedy? Does plan size matter?
Any entity, of any size, that self-insures its Rx benefits can benefit from engaging Remedy. Many types of entities – from large corporations, to regional firms, and to governments, school boards, unions and health systems – have all relied on Remedy’s people and technology to help optimize their plan and keep them ahead of market trends so they can both control spend and better manage the health of their memberships.
What is the cost to engage Remedy? How are we billed?
Remedy’s fee structure is flexible, and clients pay in several ways based on their preference (e.g. fixed fee, per claim, PMPM). Whatever method is chosen, the deliverables and pricing are fully disclosed to the client via a master services agreement and statements of work.
Are there any extra costs or hidden fees?
No, all fees are fully transparent. There are no extra or hidden fees.
Does Remedy sell directly to employers or through brokers?
Both. Whether a client comes to us directly or via a broker relationship, Remedy always works directly with the plan sponsor and its PBM to acquire the necessary information to determine the fee and execute the services.
How much time is involved from the HR/Benefits department for an initial analysis?
In order to perform our initial, no-obligation analysis, we require very little time or effort from the sponsor or its broker. To get started, we simply need a copy of the current PBM contract, a claims file and other basic plan design information, all of which can be provided to Remedy directly from the PBM. We can run a comprehensive analysis of your plan’s performance and to tell you how Remedy can help you meet your needs.